
Ebola in the DRC: between operational trial and error and scientific uncertainty
Elba Rahmouni
Rebecca Grais, Research Director at Epicentre, MSF’s epidemiology arm, and Pierre Mendiharat, Deputy Director of Operations for MSF-France, offer their insights on the Ebola outbreak in North Kivu Province in the eastern Democratic Republic of the Congo (DRC). This joint interview in four parts (the outbreak, social context, treatments, and vaccination) aims to show how science and practice interact around each outbreak.
Part 1: The outbreak
When did the outbreak in North Kivu Province begin? Did the official declaration come quickly enough?
Rebecca Grais: The first cases apparently started in April. An outbreak of Ebola virus disease was declared on 1 August 2018, after probable cases were confirmed by blood testing at Kinshasa’s Institut National de Recherche Biomédicale (INRB) on 28 July. The authorities can’t be faulted for the delay in declaring the outbreak, because it’s unrealistic to think it could have been done quickly. Having new cases appear and detecting them are two different things. To identify the virus, people have to be ill and identified as such. Yet some viral illnesses have long incubation periods (more than a week) and nonspecific initial symptoms (fever, headache, etc.). You don’t immediately think of Ebola when someone has a fever. Often, unfortunately, a number of people have to die before the alarm gets pulled.
What makes the Ebola virus even more complicated is that it is endemic in the Democratic Republic of the Congo. This is the DRC’s tenth outbreak, or episode, to date, and the second this year (after the outbreak in Equateur Province). It is really hard to predict where the virus is going to show up. I would note that we’re getting better and better at detecting such episodes.
Is this a significant episode? How is it evolving?
Pierre Mendiharat: The outbreak in West Africa from December 2013 to March 2015 was extraordinary in terms of the number of cases. Although smaller in scale thus far, the current outbreak is already significant in the history of outbreaks in the region. As of today, 23 October 2018, there are 237 cases. The outbreak has spread geographically to the region’s towns and cities: Mangina, Beni, Butembo, and Tchomia. As in the big West Africa outbreak, the virus has spread to several densely-populated cities (with 50,000, 100,000, and 200,000 inhabitants – even 600,000 in the case of Butembo) two-hours’ drive apart. Mangina was the primary focus at the start of the outbreak, but now Beni has the most new cases. The initial cases in Butembo and Tchomia came from Beni, and Beni also has the most cases lost to follow-up.
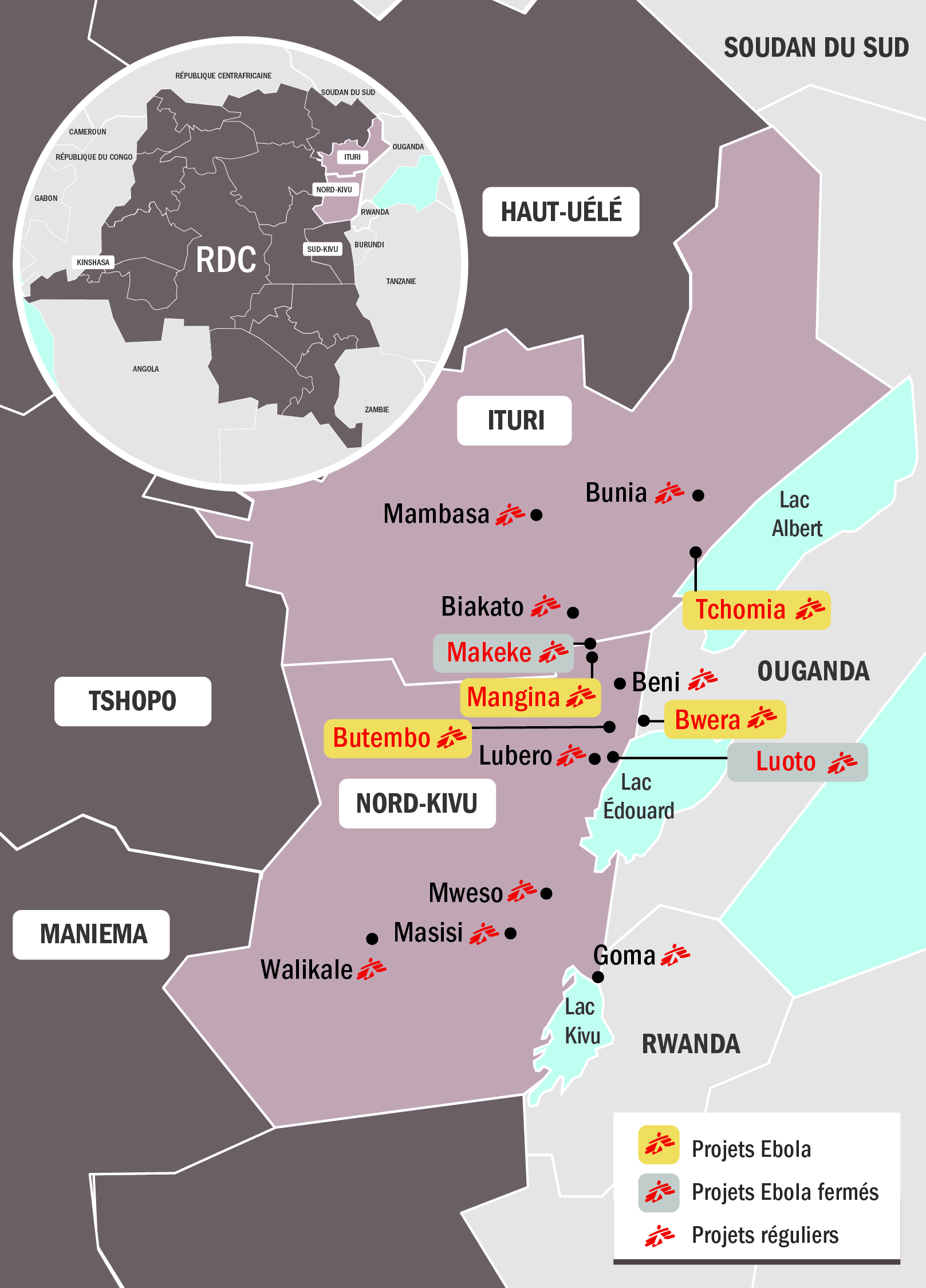
Map of MSF Ebola projects
Remember that there have been clashes between armed groups in the region for decades. There were new attacks in Beni recently – attributed to ADF (Allied Democratic Forces) rebels – resulting in “ghost town” operations that have paralyzed the cities (closing schools, government offices, and markets, stopping motorcycle taxis, etc.). These conditions make it very hard for teams engaged in contact tracing, vaccination, awareness-raising, and disinfecting Ebola Treatment Centers (ETCs) and contaminated houses to do their work. During the last ghost town operation in Beni, which lasted five days, the number of contacts traced fell from 80 to 40. That is very worrying in terms of our ability to control or stem the spread of the outbreak.
We are currently far from the end of this outbreak. In addition, the idea that an outbreak is ebbing is always difficult to handle. We saw this in West Africa; there were times when the number of cases rose, then fell, then rose again. It only takes one case to start a whole new chain of transmission. So we never really know where we are; only in hindsight can we say that we were at the end of an episode (to use Rebecca’s terminology).
Which actors are working on this episode?
Pierre Mendiharat: It’s remarkable and reassuring that mere weeks after the outbreak was declared there are so many actors so highly mobilized in this relatively remote, conflict-ridden region. There has been a sizeable deployment of experienced Ministry of Health managers from the national and regional levels and from neighboring provinces. After its failure in West Africa and reorganization of its emergency operations department, the WHO was able to mobilize large teams as soon as the outbreak started. Its actions have been very positive. There are a few other organizations that developed expertise through their work toward the end of the West Africa epidemic, as well: ALIMA, UNICEF, Save the Children, International Medical Corps (IMC), the Red Cross (for burials, in particular), the US Centers for Disease Control and Prevention… and MSF.
Rebecca Grais: That impressive mobilization is essential if we hope to control the outbreak, but it does raise some questions, since we are prioritizing this disease over others. It is a unique mobilization that can’t be generalized to other diseases.
Commentary: Why such a large-scale response to Ebola virus disease?
Rony Brauman: Unlike viral illnesses transmitted via the oral route (e.g., measles), Ebola requires direct contact with body fluids, and thus is not so easily spread. It kills far fewer people than heart disease or diabetes, for example. At MSF, however, our action does not correlate directly with demographic data like the number of deaths. What makes Ebola so frightening is that it’s a contagious disease with a very high case fatality rate (approximately 50%). Like AIDS, Zika, and other viral illnesses, Ebola is a public safety issue because it is particularly threatening in a world of global travel.
Jean-Hervé Bradol: From an historical standpoint, Ebola is reminiscent of the deadly major epidemics (plague, smallpox, cholera, Spanish flu, etc.) that slowed world population growth from the fourteenth to the eighteenth century. True, the number of Ebola cases during an outbreak is nowhere near that of the major epidemics (there were about 11,000 deaths during the large outbreak in West Africa, compared to the fifty to a hundred million deaths from the Spanish flu near the end, and in the immediate aftermath, of World War I). But as Rony points out, a case fatality rate – the percentage of cases that die – of 50% seems like a terrifying threat in a situation where person-to-person transmission is much higher. In terms of controlling outbreaks, the one in West Africa gave us an opportunity to explore, on a small scale, what to do if the number of cases explodes in spite of having taken major action at the beginning of an outbreak in an attempt to halt its spread. Generally speaking, our only strategy for outbreaks is to “nip them in the bud.” In that sense, the time and effort we devote to each outbreak are necessary if we hope to develop new strategies for dealing with another large-scale epidemic.
Part 2: The social context
There have been a number of violent reactions against health teams, most notably in Beni (throwing rocks at cars, burning health centers, etc.); why such reactions among the populace?
Pierre Mendiharat: Such violent reactions are understandable in a context of fear. The fear of being infected and of dying can cause distrust toward health workers. Some people hide or decide to travel because they don't think going to an ETC is the best way to survive. That fear is not irrational, because the mortality rate at the ETCs is indeed extremely high and health centers are generally places with increased transmission. In addition, there are all kinds of strange rumors about the disease having to do with body fluids – blood, in particular – and belief in occult forces.
It is also worth noting that the outbreak is occurring in an extremely tense general political environment; the presidential elections have been postponed several times and the central government in Kinshasa is considered less legitimate than ever. In North Kivu – a province traditionally opposed to the central government – there is a reaction of distrust that is political in nature. This is reflected, in particular, in the rumors that we’re hearing. There is one rumor, for example, that getting “flashed” by an infrared thermometer (which are everywhere, at all the crossing points) will make you vote for the government. As in all epidemics, the challenge for the authorities is to prove they are capable of responding – an obvious mixture of politics and health. In that context, a response divorced from politics is impossible.
Rebecca Grais: What we should be asking ourselves is not why there are such reactions, but where our expectation that things will go well comes from. I don’t think it’s a realistic expectation. Why should things go well? Why should people follow? It’s a frightening, deadly disease we know little about; we have little to offer and we’re asking painful things of people. In previous outbreaks, for example, imams and priests weren’t allowed to see the sick people. Families were asked not to touch patients and to bury their loved ones in an unacceptable way. We shouldn’t underestimate that human dimension. And added to that, in a context where the State no longer functions, is the lack of trust in the medical system.
There’s a political dimension at the international level, as well. The financial, reputational, and bioterrorism-related security challenges are garnering significant media coverage internationally. Even a small-town newspaper in Pennsylvania will cite the number of Ebola cases in the DRC. All this is causing an unusual amount of pressure in an already tense political context.
Given these reactions, what information and education activities do patients and their families need? What attention are patients receiving?
Pierre Mendiharat: The Ministry of Health has primary responsibility for health promotion activities. But at our level of operation, we also have messages for patients, their families, and health workers at the ETCs and within our health center disinfection and decontamination activities. Formulating messages in the best possible way to correctly explain something that is very scientifically complicated, and that we don’t know a lot about, to the populace is really hard. Not to mention translation problems, which make understanding the messages even harder.
Regarding the attention given to patients and their loved ones, we’ve made a lot of progress compared to the West Africa outbreak. All of the ETCs can be seen from the outside. The notorious “safe” burials are now called “safe and dignified burials” and, practically speaking, the people in charge of that activity strive to ensure safety while at the same time respecting the families and their desire for a ceremony that allows them to begin mourning. That activity is still difficult, however. Burials often take place the day after death; when someone dies outside a health center, a team must be sent very quickly to test whether the person died of Ebola and, if so, to ensure appropriate burial conditions. Unfortunately, due to organizational problems, people are still being buried in ways unacceptable to their families or without having a sample taken.
Rebecca Grais: We have to find a way to offer these simple, universal things (family contact, decent burial, etc.) that every patient is entitled to. There’s nothing extraordinary about these improvements; they are often just common sense, but are not easy to implement in the complicated context of an outbreak.
Part 3: Treatments
What different types of treatment are available? Do all patients receive treatment?
Rebecca Grais: This is not a typical treatment situation; indeed, the efficacy of the drugs being offered has not been confirmed scientifically. There are five such drugs; three are monoclonal antibodies (ZMapp, mAb114, and REGN3470-3471-3479) and two are antivirals (remdesivir and favipiravir). ZMapp is the best known internationally. MAb114 comes from the serum of a person who survived the 1995 Kikwit outbreak in the DRC. As a result, there is a sense of ownership by the Congolese health officials, an important nationalist dimension to that drug, even though – like the other antibody treatments – it was developed in the United States. With the exception of favipiravir, all of these drugs were originally designed by the military for fighting bioterrorism. After that they were developed in slightly different contexts: mAb114 in the public sector and ZMapp in the private sector, with help from a Canadian biotech firm. Remdesivir was originally developed not for Zaire ebolavirus, but for any filovirus.
We know very little about the virus itself or about the treatments. What’s important in this context – where patients are at high risk of death and we don't have the comfort of being able to say that the treatments work (though we do know, a priori, that they are well tolerated) – is to offer the patients treatment. It’s a medically ethical approach, where the treatment is presented as an option: “this treatment is available and if you want to take it we are ready to give it to you, but we have no idea how effective it is.” The use of drugs requires a protocol and informed consent from the patient. Having the option of offering drugs in development is already a big improvement compared to previous outbreaks.
Pierre Mendiharat: We decided not to say “experimental treatment” in our public statements, out of fear it would be misinterpreted – as if the patients were the guinea pigs for our experiments. We prefer to say “drug in development.” But the vast majority of patients and caregivers want to use the drugs. There is hope that they will work and, to be frank, the only way to know whether they work is to use them. And because the mortality rate is extremely high without treatment, there isn’t much to lose with treatments that at least won’t make the patient worse.
What is MSF’s relationship with the local officials regarding the treatments?
Pierre Mendiharat: What’s happening in the field is very positive; for the first time, within a few weeks of the outbreak being declared, every patient identified through testing was offered treatment. Even so, the relationship was complicated; there were differences of opinion, due in particular to the number of drugs available, each having its own specific characteristics. Without any data, it’s hard to agree on the choice of treatment. When things are not clear, individual and collective intuitions collide. The WHO has developed an algorithm and is coordinating a collective decision-making mechanism for determining which drug to administer to each patient, though it should be up to the clinician to decide as a last resort.
In August, the Ministry of Health decided to administer mAb114 to ten infected staff members (and to other patients since then). The ten patients survived. While these are very small numbers, the Ministry of Health seems to have done the required lab testing around these patients. Generally, MSF is having trouble getting access to the patients’ follow-up lab data for this outbreak. We don’t have our own ETCs; we work in ETCs run by the Ministry of Health, which controls the laboratories and doesn’t want to share the data with us, apparently out of fear that we’ll use it before they do in a scientific publication. We are impatiently awaiting the results from their studies.
Rebecca Grais: There’s a desire on the part of the different actors to demonstrate the efficacy of the drugs. That hasn't always been the case in the past, so that’s progress. But I doubt that the Ministry of Health is capable of “proving” the efficacy of mAb114. On the other hand, and it’s a first step, they are going to show that the treatment hasn’t killed anyone, that it’s something that should be pursued and left to languish… And then they’re going to be able to find a manufacturer.
While there are more drugs available for this outbreak, is enough being done in terms of basic clinical care, that is, symptom management?
Rebecca Grais: That’s a hard question. When people are dying, there is never enough being done. How we treat patients, how we develop relationships with their families, the logistical aspects…all that is important. What we can say is that this time around the participants are concerned about basic clinical care (rehydration, pain management, etc.), and that alone is a major improvement.
Pierre Mendiharat: We’re still far from being capable of basic intensive care; there's the constraint of protective equipment, the difficulty drawing blood and administering infusions safely, etc. We have tried to develop basic intensive care by better monitoring lab tests and having centers better adapted to that kind of monitoring and to monitoring patients visually. On the whole, however, we haven’t made significant progress in that regard. The isolation cubes developed by ALIMAVideo: Ebola in the DRC: ALIMA opens a treatment center equipped with CUBEare certainly a good way to improve patient care. The medical institutions have made further progress on the treatment question.
Part 4: Vaccination
What is the vaccination strategy?
Rebecca Grais: It should be noted that the vaccine being used (rVSVDG-ZEBOV-GP) is not yet registered and its clinical efficacy has still not been established. Its use is one part rationality and one part uncertainty; hence the importance of obtaining informed consent of the people being vaccinated. Vaccination is done by the Ministry of Health with WHO support. What is truly new is its large-scale use; sixteen thousand people have already been vaccinated. The strategy being used, called “ring vaccination”, vaccinates everyone who had contact with a patient (contacts), as well as all of their contacts (the contacts’ contacts). In addition, there are frontline workers (FLWs) and people who go to the vaccination sites because they want to be vaccinated. In reality, it’s often difficult to adhere to this strategy for security reasons.
Pierre Mendiharat: The question of which vaccination strategy is best is – for me – far from settled. There is the ring strategy, but also another strategy that vaccinates by geographic area. In Equateur, for example, they vaccinated entire small villages without any selection process, and that choice turned out to be appropriate for controlling the outbreak's spread. In a context of heightened insecurity, for districts that we don’t have ready access to, like in Beni, it should be possible to have all of the health workers come to us for vaccination (whether they’ve had contact with Ebola patients or not). Generally speaking, if there’s an outbreak, and since we have bet, as an organization, that vaccination is protective, I think it’s better to do more of it, rather than less. I also see this new vaccine as a great opportunity to control the outbreak since – by giving us something to offer them – vaccination helps us monitor contacts.
Is MSF international staff being vaccinated?
Pierre Mendiharat: Except for national personnel who were vaccinated during the previous outbreak in Equateur, almost no MSF frontline personnel were vaccinated during the first two months of the outbreak. Either the vaccine wasn’t offered, or it was presented in such a negative way that no one wanted to get vaccinated. According to the protocol for health workers, everyone must be informed about the vaccine before they start working in an Ebola operation, and it must be offered to all frontline health workers (upon arrival in the zone for international staff, since the vaccine is not yet available in France). It seems that practice is finally in sync with theory, and some have now been vaccinated, along with most of the members of the hospital hygiene staff.
There were negative messages about the vaccine for practical reasons, as well. Twenty-five to thirty percent of those vaccinated develop a fever in the first 24 to 72 hours. For expatriates who are only going to be in the field for a month, being out of commission for the first few days is a drawback. However, the institution cannot make the decision for individuals or prioritize operations over prevention.
Rebecca Grais: That some people believe the vaccine works and others believe it doesn’t is not what’s important. The main thing is to give accurate information and let people choose.
Pierre Mendiharat: Some people at Médecins Sans Frontières argue that since we don’t know for sure how well the drugs and vaccine work, what’s really important are the six pillars laid out a long time ago for controlling the spread of Ebola1: Monitor the evolution of the disease and the emergence of new foci; 2: Educate the community about the disease, how to avoid it, and what to do if confronted with it; 3: Set up treatment centers that permit patient isolation and care; 4: Identify and trace patient contacts; 5: Ensure that burials do not cause new infections; 6: Help health care facilities with infection control infection to prevent the disease from spreading, while continuing to provide care to the community. 5 minutes pour comprendre Ebola en zones de conflits [Five minutes for understanding Ebola in conflict zones] (video in French). Others readily agree that the six pillars are essential, but feel that vaccination is an equally-important seventh pillar. It’s less obvious for treatment, since treating a patient (or not) has no direct impact on the spread; although again, offering treatment in the ETCs might change how the populace perceives them, and we now that having people go to the ETCs helps limit the spread of the virus, in that patients are confined there.
Regarding treatments and vaccination, is it possible to do science during a crisis?
Rebecca Grais: Not only is it possible to do studies during a crisis – it’s necessary. We’ve been gathering information since 2014. In some ways, it was thanks to the West Africa outbreak that we were able to develop the drugs and vaccine. We were just starting to use them as the outbreak was ebbing, but without that, we wouldn't have anything today.
The fact that there are five treatments raises a lot of questions. Which works best? According to what criteria? Which is easiest to administer? Which takes effect most quickly? Which is easiest to store? Et cetera. Conducting studies in this type of context (as MSF and Epicentre do) is what allows us to document what will be possible in the future.
Pierre Mendiharat: With each outbreak we acquire new knowledge and make progress. Beyond the difficulty of doing science during a crisis, the challenge is continuing to do it between outbreaks. We really should be doing much more during the calm periods, knowing that once an episode starts, everything happens very quickly. A research protocol can't be put together in a few weeks.
Rebecca Grais: We have to flip how we think about it; stop thinking that outbreaks are something rare and start showing an ongoing interest in the family of filoviruses responsible for Ebola and Marburg hemorrhagic fever. Beyond the medical response, Ebola virus disease – in crystallizing a whole raft of difficulties – poses the general question of our capacities and our investment. From that emerges a host of questions, like, for example, our work priorities, our desire to position ourselves as a leader or a follower on a given subject, and also the issue of training our doctors so that they’re prepared before a new outbreak occurs.
To cite this content :
Elba Rahmouni, “Ebola in the DRC: between operational trial and error and scientific uncertainty ”, 26 octobre 2018, URL : https://msf-crash.org/en/blog/medicine-and-public-health/ebola-drc-between-operational-trial-and-error-and-scientific
If you would like to comment on this article, you can find us on social media or contact us here:
Contribute



Commentaires
merci pour cet article.
Super article, bravo
Je suis un resident de Beni
Juste savoir les mesures post covid entretenues dans cette ville de Beni,
quelle stratégie de prevention gardée au quotidien au sein de la population de Beni.
L'ideal serait de poursuivre avec des seances de sensibilisation mediatique par de spots radiodiffusés, des affiches et prospectus geant au travers les quartiers precaires de la ville et les entrees principales.
Ce qui est etonnable, c'est de voir cette nostalgie qu'affiche la population de Beni gardant en tete la maladie a virus ebola comme un boom pecuniaire qui a marqué la ville , qui pour les vehicules en location, qui pour les boites de nuit, terasses, les malewas, les restaurants, le boom immobilier, hehhh, le vieux metier du monde etait florissant a en croire à la nostalgie de la tranche des beneficieres de la ville et des quariers et points chauds de la ville (Matonge, triangle de la mort, Le Troc, Ishango, Tapis Rouge, HB), au finish, hheeehh, l'OMS a endossé ce debordement des moeurs.
Ce qui est etonnable en plus, j'etais dans une terrasse entrain de suivre le match que jouait les leopards de la RDC, l'equipe nationale sur le boulevard Nyamwisi, à l'annonce du dernier cas de 2021 recent, j'ai vu comment les filles souhaient voir cet episode susciter une occasion de boom financier dans la ville, Dieu merci ca n'a pas eu de l'ampleur au regres des personnes qui en font un business
Merci, Jose
Add new comment