OFF THE CUFF is a participative blog run by the Crash. Its purpose is to expose the diversity of experiences and opinions that exist among humanitarian aid practitioners. Online comments as well as direct contributions are more than welcome.
Views expressed on this blog are those of their authors and do not necessarily reflect the official positions of Médecins Sans Frontières
Humanitarianism in the Modern World. The moral economy of famine relief
“Humanitarianism in the Modern World. The moral economy of famine relief” published by Cambridge University Press, is an open access book written by a team of three people, whose aim is to provide a history of contemporary humanitarianism through the prism of famines. Norbert Götz, Georgina Brewis and Steffen Werther are treading on fertile ground, as the number of publications on the history of humanitarianism has multiplied in recent years. However, the contribution they present here is rich and original.
Médecins Sans Frontières and Humanitarian Negotiations for Access in the Democratic Republic of the Congo
Myfanwy James is a research fellow at the London School of Hygiene and Tropical Medicine & DPhil (PhD) graduate from the University of Oxford. In this video, she presents her thesis entitled: “Instruments of Identity: Médecins Sans Frontières and Humanitarian Negotiations for Access in the Democratic Republic of the Congo (RDC)”.
Covid-19 Reading List : the vaccines special edition
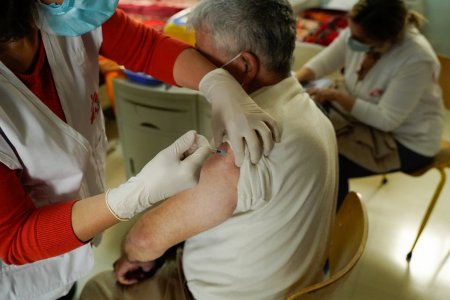
We can all agree that the emergence of Covid-19 vaccine is “an absolutely astonishing development”, but vaccines are unlikely to completely halt the spread of the virus, let alone eradicate it. Yet even without achieving herd immunity, the ability to vaccinate vulnerable people seems to be reducing hospitalizations and deaths from Covid-19.
The “disappeared” of Congo-Zaire, 1996-1997. The question of the massacres of Rwandan Hutu refugees in the Democratic Republic of Congo
There is a new book out by Patrick de Saint-Exupéry entitled La traversée. Une odyssée au cœur de l’Afrique [The crossing. An odyssey in the heart of Africa]. What odyssey? Crossing the Congo (Zaire, later the Democratic Republic of Congo) from Rwanda. The author describes his encounters, the beers he had here and there, the bumpy rides on the back of a motorcycle (to Kisangani), a trip down the Congo River, flying over the dense forest on his way to Mbandaka.
Ebola and innovation: examining the approach to the Nord Kivu epidemic
Within four months of the first notification of Ebola cases in August 2018, the Nord Kivu (and Ituri) Ebola epidemic had become the second-largest on record. Notwithstanding a rapid and massive mobilisation of resources, the outbreak continued beyond the most pessimistic predictions and the case fatality rate (the proportion of people with the infection who die from it) remained static at 66%. Despite numerous lesson-learning exercises following the Ebola epidemic in West Africa in 2014–2016, and despite the development of new vaccines and treatments, after 3,444 cases and 2,264 deaths it is difficult to claim that outcomes are better this time around.
Nursing homes and their ghosts: MSF's experience in France during the Covid-19 health crisis
This article was published in Mouvements magazine on March 24, 2021. In the early spring of 2020, the humanitarian organization Médecins Sans Frontières (MSF) launched a mission in nursing homes in the Ile-de-France region, which had been hit hard by the Covid-19 pandemic. After considering the implementation of night-time palliative care, the organization finally decided to provide daytime support to the nursing homes in difficulty. Once the crisis was over in the summer, the MSF teams started offering mental health support to nursing home staff. A look back at this experience on September 28, 2020 with four members of the mission, Olivia Gayraud (project coordinator), Jean-Hervé Bradol (M.D. and CRASH1 member), Marie Thomas (psychologist) and Michaël Neuman (CRASH coordinator).
What to think, do and say about the Covid-19 vaccination?
Blog written by Jean-Hervé Bradol, director of studies at the Crash.
Today, in order to obtain supplies of vaccines against Covid-19, there is neither a major difficulty related to price, nor a major obstacle related to intellectual property rules, nor a deficit in bio-medical research. However, these three topics are generally at the heart of MSF's communication in the area of access to medical care for those in most need. Our discourse must therefore evolve.
With the emergence of worrying variants of the virus present in the early stages of the pandemic and, as a consequence, the need to vaccinate on a global scale as quickly as possible, the world is facing a double challenge: biological engineering and ultra-industrial production – “ultra” echoing the need to produce on a global scale in a short period of time.
Should we discriminate in order to act? Profiling: a necessary but debated practice
In this article for the Humanitarian Practice Network, head of the Research Unit on Humanitarian Stakes and Practices (UREPH) for MSF Geneva Françoise Duroch and Crash director of studies Michaël Neuman discuss the implications and reasons behind the growing practice of staff profiling for MSF.
In October 2020, MSF organised a workshop in Dakar on staff profiling in operations in the Sahel. Profiling involves the selection of staff based on non-professional criteria, including nationality, skin colour, gender and religion. As such, it raises a number of ethical and practical concerns. As a result of profiling, US nationals have not been deployed in MSF operations in Colombia because of the risk of kidnapping, and Chadians and Rwandans have been excluded in the Central African Republic and eastern Democratic Republic of Congo respectively, because of regional conflicts. The use of profiling has increased in recent years in West Africa, as the threat of kidnapping of Westerners by radical jihadist groups has intensified.
A “partnership” experience, A guided reading of Che Guevara's diary in Congo
Operational partnerships between two organisations are a practical approach to humanitarian responses. MSF considers such partnerships when the objective it is pursuing in a country is similar to that of an existing national organisation, and when there is potential for synergy between these two entities. I would like to take a bit of a detour by looking at an experience that is in some ways similar: when Che Guevara tried to lead the revolution in Congo - Zaire by supporting the organisation of the guerrilla movement in the east of the country.
Afghanistan : Should MSF accept the risk of targeted killings?
The May 12th massacre at the MSF-supported maternity hospital in Dasht-e-Barchi (Afghanistan) raises, yet again, the question of our limits with regard to risk. What is an acceptable level of danger for humanitarian aid workers? How do we set limits? Why would MSF decide to leave Kabul but remain in Herat, for example, or leave Afghanistan but remain in Niger, Burkina Faso, Mali, or Somalia, where the teams also face extreme danger?
Communicating and convincing: a humanitarian perspective on the French response to the coronavirus epidemic
In this paper, the two authors examine certain aspects of the French response to the epidemic in the light of the experience of Médecins Sans Frontières (MSF) in that field, primarily with respect to the relationship between the actors of the response and the beneficiaries.
Covid-19 Reading List - Part 4
After a few months of respite the coronavirus epidemic has resumed its spread. With the second wave becoming a reality in many European countries, the Crash team decided to share some recent reading on the biomedical, political and social aspects of the pandemic in an attempt to shed some light on this tragic Season 2. As in previous editions, some articles are in English and some in French, and they are taken from both mainstream and specialist sources.